A One Health program is crucial for preventing zoonotic spillover
- Rapid Detection and Diagnosis: A high index of suspicion among medical professionals, coupled with advanced laboratory infrastructure like the National Institute of Virology (NIV) unit in Alappuzha, ensures early case identification.
- Efficient Containment: The state machinery excels at swift contact tracing, quarantining, and implementing infection control protocols in hospitals, effectively breaking the chain of human-to-human transmission.
- Effective Public Communication: Timely and transparent communication helps manage public fear, dispel misinformation, and ensure community cooperation.
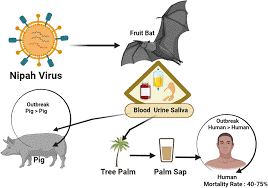
- High Human Cost: Nipah has a high case fatality rate (40-75%), meaning lives are invariably lost before the outbreak is controlled.
- Socio-Economic Disruption: Each outbreak leads to localised lockdowns, restrictions on movement, and trade embargoes on agricultural produce, causing significant economic distress and social anxiety.
- Strain on Healthcare Resources: Managing a Nipah outbreak diverts immense financial and human resources, putting a severe strain on the healthcare system.
- Surveillance of Bat Reservoirs: A systematic, year-round surveillance program is needed to map bat colonies, study their migration patterns, and monitor the prevalence and shedding of the Nipah virus within these populations.
- Habitat Protection: Deforestation and habitat destruction force bats into closer proximity with human settlements, increasing the chances of contact. Conservation efforts are, therefore, a public health imperative.
- Climate Change Impact: Research is needed to understand how changing climate patterns may affect bat behaviour, diet, and viral shedding, potentially creating new hotspots.
- Intermediate Host Surveillance: While direct bat-to-human transmission is common in India, the role of intermediate hosts like pigs (as seen in Malaysia) cannot be ignored. Regular surveillance in domestic animal populations is crucial.
- Promoting Safe Practices: Farmers should be educated on securing livestock from bat exposure and protecting wells and water sources from contamination by bat droppings.
- Targeted Awareness Campaigns: Public awareness must go beyond outbreak periods. Communities in high-risk zones need sustained education on avoiding half-eaten fruits, handling bats found in homes or wells safely, and recognizing early symptoms.
- Strengthening Primary Healthcare: Primary Health Centres (PHCs) are the first point of contact. Training primary care doctors and health workers to identify febrile illnesses with neurological symptoms is critical for early detection.
- Inter-sectoral Coordination: A permanent, empowered state-level committee with representatives from the Health, Forest, Animal Husbandry, and Revenue departments must be established. This body should be responsible for overseeing surveillance, research, and prevention activities continuously, not just during outbreaks.
- Funding and Research: Greater investment is needed in indigenous research for developing vaccines, monoclonal antibody therapies, and rapid, point-of-care diagnostic kits.

